LABORATORY ACCIDENTS
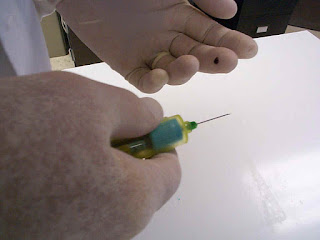
Laboratory Accidents DEFINITION · Laboratory accident- Incidences and disasters which occurs in the Laboratory (occupational hazards) · Management of Laboratory accidents-pertains to how disasters are handled with the aim of preventing them from reoccurring. · Complaint- Client protest on Laboratory Services · Process deviations- Making short cats, moving away from standard procedures · Instrument problems-Problems resulting from Instrument not functioning well · Occurrence log- A register or form in which all laboratory incidences are recorded · Aerosol, i.e. Infected airborne droplets, into the atmosphere consisting of bacteria...